<2>A 15 year-old boy from Mexico presents with chronic renal failure . A careful history obtained from his uncle indicates that he has not been treated with dialysis. Radiography of the hand and forearm demonstrates erosion of the terminal phalanges and marked metaphyseal resorption of the ulna and radius. Excessive secretion of which of the following hormones most likely contributed to these problems? A. Aldosterone B. Calcitonin C. Parathyroid hormone D. Renin E. Vitamin D Answer
<3>Which of the following substances takes part in the nonoxidative killing pathway by which pathogenic bacteria can be killed? A. Hydrogen peroxide B. Hypochlorous acid C. Lysozyme D. Myeloperoxidase E. Superoxide ions Answer
<4>An adolescent male is referred for drug abuse. He confides to the therapist that he has been taking large amounts of "reds" (secobarbital sodium) for some time, and that they make him feel confident and calm. He would like to try to stop and says he would like to "do it on his own," without additional medication. The therapist should advise the patient to detoxify with medical assistance because of the danger of A. insomnia B. rebound anxiety C. recidivism D. respiratory depression E. seizures Answer
<5>A neonate develops bile-stained vomiting and progressive abdominal distention, and does not pass meconium over the first two days of life. The anus is patent, and the bowel loops are palpable. Plain radiograph shows bubbly meconium in the right lower quadrant. No localized areas of constriction or other abnormalities are noted. Which of the following is most likely etiologically related to this infant's condition? A. Cystic fibrosis B. Hirschsprung's disease C. Meckel's diverticulum D. Omphalocele E. Polycystic kidney disease Answer
<6>A 33-year-old newlywed presents to her physician with a sharp, burning epigastric pain. She had recently begun a regimen of non-steroidal antiinflammatory agents to help relieve pain caused by rheumatoid arthritis. Her physician recommends misoprostol to relieve her gastric distress. Before prescribing this drug, the physician should first obtain the results of a(n) A. antinuclear antibody test B. barium swallow C. esophageal manometry D. osmotic fragility test E. pregnancy test Answer
<7>A medical student examining a patient is startled when he cannot "find" the patient's heart during auscultation. The patient laughs and tells him to "try the other side." Auscultation on the right side of the chest does demonstrates an apparently normal heart beat. Further physical examination demonstrates that the liver edge can be palpated on the left but not the right side of the abdomen. Questioning of the patient about his medical history reveals a history of bronchiectasis and sinusitis. Which of the following should be suspected? A. Down syndrome B. Kartagener syndrome C. Kawasaki disease D. Marfan syndrome E. Turner syndrome Answer
<8>An 82-year-old man develops a round, fluid-filled cystic structure on the back of his knee that limits the knee's mobility. This most likely represents an enlargement of which of the following structures? A. Deep infrapatellar bursa B. Prepatellar bursa C. Semimembranous bursa D. Superficial infrapatellar bursa E. Suprapatellar bursa Answer
<9>A 27-year-old male presents to the doctor with complaints of "heartburn" and painful, sour-tasting acid reflux that has not been alleviated by over-the-counter medications. An endoscopic exam is performed and a biopsy of the distal esophagus is taken. Microscopic examination of the tissue shows normal tissue without pathologic changes. What type of mucosa is normal for the distal esophagus? A. Ciliated, columnar epithelium B. Keratinized, stratified, squamous epithelium C. Non-ciliated, columnar epithelium D. Non-keratinized, simple, squamous epithelium E. Non-keratinized, stratified, squamous epithelium F. Pseudostratified, columnar epithelium Answer
<10>A 35-year-old construction worker is complaining of aching pain in his right hand since starting a new project in which he has been operating a jack hammer for several hours a day. At first the pain was tolerable, but now he awakens at night and has recently noticed numbness and tingling in his hand. He continues to perform his daily work despite his symptoms. On physical exam, there appears to be decreased sensation over the first three-and-a-half digits in the right hand. Which muscles are likely to be affected in addition to the sensory loss? A. Abductor digiti minimi and 1st and 2nd lumbricals B. Abductor digiti minimi and 1st through 4th dorsal interossei C. Abductor pollicis brevis and opponens pollicis D. Wrist extensors E. Wrist supinators Answer
<11>A pediatrician discovers a large mass in the abdomen of a 3-year-old child. Ultrasound examination demonstrates that the mass appears to arise from the right kidney. Which of the following tumors is most likely present? A. Cortical adenoma B. Hemangioma C. Nephroblastoma D. Oncocytoma E. Renal cell carcinoma Answer
<12>A knife wound to the face selectively damages the facial nerve. Salivation from which of the following would be impaired? A. Parotid and sublingual glands B. Parotid and submandibular glands C. Parotid gland only D. Sublingual gland only E. Submandibular and sublingual glands F. Submandibular gland only Answer
<13>Molecular studies on an abdominal lymph node containing lymphoma demonstrate t(2;8)(p12;q24) translocation. This is most compatible with which of the following diseases? A. Burkitt's lymphoma B. Mantle cell lymphoma C. Multiple myeloma D. Small cell lymphoma E. Small cleaved cell lymphoma Answer
<14>A patient with long-standing constipation enters a clinical research study. After a complete physical examination, a small intraluminal balloon is inserted through the anus to the rectum. Transducers are also inserted to measure internal and external anal sphincter pressures. Inflation of the rectal balloon causes the external anal sphincter to contract, but the internal anal sphincter, which exhibits normal tone, fails to relax and the urge to defecate is not sensed. Which of the following structures is most likely damaged? A. Internal anal sphincter B. External anal sphincter C. Pelvic nerve D. Pudendal nerve E. Rectum Answer
<15>A very ill-appearing 64-year-old woman is admitted to the hospital with malaise, fever, and low-back pain. Funduscopic examination on admission was unremarkable, but one day later, multiple small white spots surrounded by hemorrhage are observed on both retinas. The ophthalmologic findings suggest which of the following diagnoses? A. Bacterial endocarditis B. Crohn's disease C. Diabetes mellitus D. Glaucoma E. Urosepsis
<16> A 52-year-old man is admitted to the hospital complaining of chest pain and difficulty breathing. He has a history of rheumatic valvular disease. Physical examination reveals a systolic murmur. Pressure tracings from the aorta, left ventricle, and left atrium are shown in the diagram. This patient is suffering from which of the following? A. Aortic obstruction B. Aortic regurgitation C. Infarction of the left ventricle D. Mitral obstruction E. Rupture of the chordae tendineae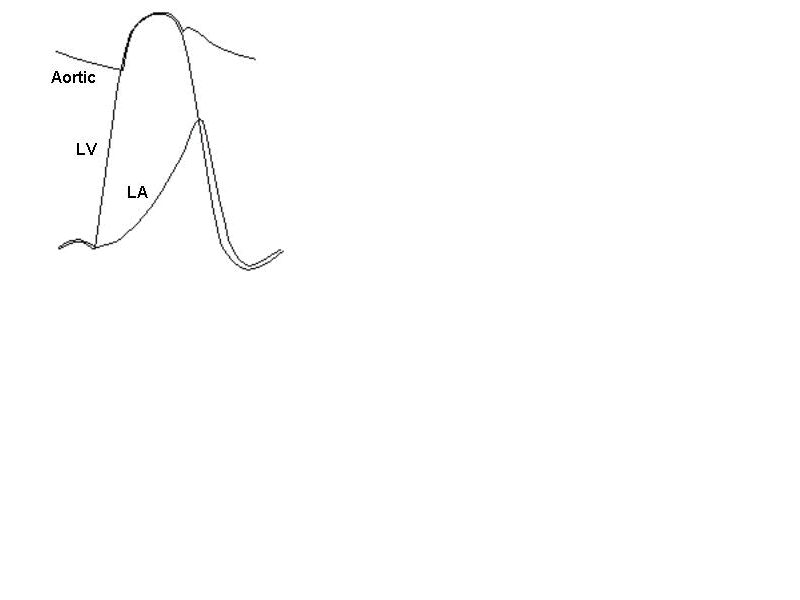
<17>A 79-year-old man complains of pain in the upper portion of his neck on swallowing. He occasionally regurgitates undigested food shortly after eating. Which of the following is the most likely etiology of his problems? A. Mallory-Weiss tears B. Plummer-Vinson syndrome C. Schatzki rings D. Traction diverticula E. Zenker's diverticulum Answer
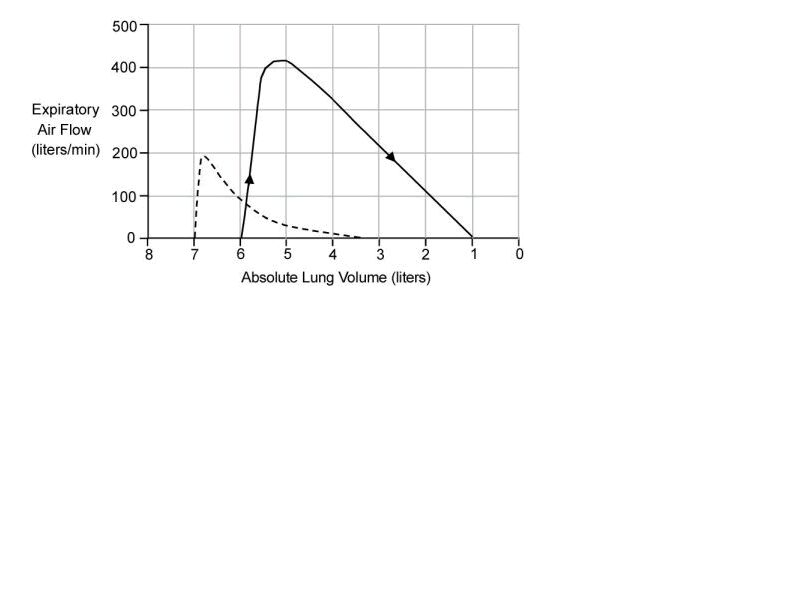
<18> The diagram above shows maximum expiratory flow-volume (MEFV) curves from a typical healthy individual (solid curve) and from a 62-year-old carpenter who complains of shortness of breath (dashed curve). The carpenter most likely suffers from which of the following disorders? A. Asbestosis B. Emphysema C. Pleural effusion D. Pneumothorax E. Silicosis Answer
<19>A newborn baby is noted to have a left unilateral cleft lip. There are no abnormalities of the baby's palate. Which of the following developmental defects accounts for this occurrence? A. Failure of the left lateral palatine process to fuse with the median palatine process B. Failure of the left maxillary prominence to unite with the left medial nasal prominence C. Failure of the primary palate to fuse with the secondary palate D. Failure of the right and left medial nasal prominences to merge E. Failure of the right palatine process to fuse with the left palatine process Answer
<20>A 26-year-old pregnant migrant worker sustains a placental abruption, and is admitted to the intensive care unit. While in the unit, she begins bleeding from multiple sites, including her venipuncture sites and oral mucous membranes. Which of the following studies would be most valuable in assessing this patient's condition? A. Partial thromboplastin time, kininogen, and factor VIII levels B. Platelet count, fibrinogen levels, and fibrin degradation products C. Platelet count, thrombin time, and prekallikrein levels D. Prothrombin time and factor VIII levels E. Thrombin time, fibrinogen levels, and factor VIII levels Answer
<21>A 59-year-old woman with advanced, metastatic lung cancer develops profound fatigue and weakness and alternating diarrhea and constipation. Physical examination demonstrates hyperpigmentation of skin, even in areas protected from the sun. Tumor involvement of which endocrine organ is most strongly suggested by this patient's presentation? A. Adrenal gland B. Endocrine pancreas C. Ovaries D. Pituitary gland E. Thyroid gland Answer
<22>A 38-year-old construction worker presents with constant back pain that is exacerbated by movement. After being discharged from the emergency room, the man gets a prescription filled, and takes the recommended dose of the medication. After about 45 minutes, he begins to feel sleepy, has a dry mouth and can feel his heart "racing." Based on this information, which of the following drugs was most likely prescribed? A. Baclofen B. Cyclobenzaprine C. Diclofenac D. Methocarbamol E. Rofecoxib Answer
<23>A 54-year-old man develops sustained, severe chest pain. He takes several antacid tablets without significant relief. Finally he tells his wife, who demands that he go to the emergency room. At the hospital, he is diagnosed with a myocardial infarction, and is admitted and stabilized, then released several days later. Three weeks after the myocardial infarction, the man develops steady, burning chest pain. He returns to the emergency room, where a friction rub is heard on auscultation. Which of the following is the most probable underlying cause of this complication? A. Autoimmune phenomenon B. Bacterial infection C. Chlamydial infection D. Fungal infection E. Viral infection Answer
<24>A 43-year-old man presents to a urologist because of a lesion on his penis. Physical examination reveals an 8-mm opaque, gray-white, relatively flat penile plaque. A biopsy is performed on the lesion; the pathology report indicates the presence of clearly dysplastic squamous epithelium. Which of the following is the most likely diagnosis? A. Bowenoid papulosis B. Bowen's disease C. Condyloma acuminatum D. Erythroplasia of Queyrat E. Giant condyloma Answer
<25>A sexually active 25-year-old man develops epididymitis and orchitis . Needle biopsy demonstrates a prominent leukocytic infiltrate with numerous neutrophils. Which of the following organisms is the most likely cause of this man's infection? A. Escherichia coli B. Mycobacterium tuberculosis C. Neisseria gonorrhoeae D. Pseudomonas sp. E. Treponema pallidum Answer
<26> Respiratory rate 15/min Blood pressure 120/80 mm Hg Cardiac output 5 L/min Heart rate 50/min A 25-year-old man is participating in a clinical study to determine the cardiovascular response to physical exercise. Basal measurements are shown above. What is his stroke volume during resting conditions (in mL/min)? A. 50 B. 75 C. 100 D. 125 E. 150 Answer
<27> A couple has four children, three girls and a boy. The girls are healthy, but the boy develops corneal opacities, painful neuropathies , and multiple, violaceous nodules distributed diffusely over his skin. Two of the daughters marry and have a total of seven children. As shown in the pedigree above, two of these children develop the same syndrome as did the affected son in the F1 generation. Which of the following is the likely diagnosis? A. Fabry's disease B. Gaucher's disease C. Krabbe's disease D. Metachromatic leukodystrophy E. Niemann-Pick disease Answer
<28>A 37-year-old man presents to a physician because of a lesion on the shaft of his penis. On physical examination, a solitary, thickened, whitish plaque with a slightly ulcerated, crusted surface is observed. Biopsy reveals markedly dysplastic epithelial cells, many mitoses (some of which are abnormal), disordered epithelial maturation, and an intact basement membrane with no evidence of stromal invasion. Which of the following is the most likely diagnosis? A. Bowenoid papulosis B. Bowen's disease C. Condyloma acuminatum D. Erythroplasia of Queyrat E. Squamous cell carcinoma Answer
<29>A 23-year-old woman presents to the emergency room with pelvic pain. A Gram's stain of her cervical discharge reveals multiple polymorphonuclear leukocytes, but none contain gram-negative diplococci. Which of the following statements best describes the two organisms that most commonly cause this disorder? A. Both are unlikely to recur because of acquired cell mediated immunity B. Both are unlikely to recur because of antibody mediated immunity C. Both induce endocytosis by epithelial cells D. Both are obligate intracellular parasites E. Both respond to b-lactam antibiotics Answer
<30>A 64-year-old white female who was diagnosed with rheumatoid arthritis two years ago has been taking salicylates and other NSAIDs for the past 18 months without adequate relief of her symptoms. Her physician decides to institute methotrexate therapy. Over the next seven weeks she receives prednisone as a form of "bridging therapy" to help prevent pain and inflammation while waiting for the pharmacological benefits of methotrexate to begin. Which of the following is she most likely to experience secondary to her glucocorticoid therapy? A. Dehydration B. Hyperkalemia C. Hypocalcemia D. Hypoglycemia E. Hyponatremia Answer
<31>A 32-year-old construction worker arrives in the emergency room after an accident on the job. The tendon of the biceps brachii at the elbow has been severed by a laceration that extends 2 cm medially from the tendon. Which of the following structures is likely to have been injured by medial extension of the laceration? A. Brachial artery B. Musculocutaneous nerve C. Profunda brachii artery D. Radial nerve E. Ulnar nerve Answer
<32>A patient with essential hypertension is starting diuretic therapy. He has a history of calcium oxalate renal stones. Which of the following diuretics would be most appropriate to give this patient? A. Acetazolamide B. Furosemide C. Hydrochlorothiazide D. Spironolactone E. Triamterene Answer
<33>A 65-year-old man with hyperlucent lung fields develops extreme shortness of breath over a period of about 15 minutes. Chest x-ray shows a shift of the mediastinum to the right, and the lung field on the left appears even more hyperlucent than before, with the exception of a white shadow near the heart border. Which of the following is the most probable cause of the patient's current problem? A. Bronchogenic carcinoma B. Pleural effusion C. Pulmonary embolism D. Rupture of an emphysematous bulla E. Tuberculosis Answer
<34>A patient is brought to the emergency room in a coma due to diabetic ketoacidosis. Insulin therapy is begun immediately. Which of the following therapies should also be begun immediately? A. Calcium supplementation B. Creatinine supplementation C. Magnesium supplementation D. Potassium supplementation E. Sodium supplementation Answer
<35>A 69-year-old man with Alzheimer disease and a 10-year history of type 2 diabetes is brought to a family practice clinic by his daughter. The patient is unable to give a clear account of how carefully he controls his blood glucose. Which of the following laboratory parameters could be used to assess glycemic control over the past 3-6 months? A. Blood glucose B. Blood insulin levels C. Blood ketones D. Glycosylated hemoglobin E. Urinary glucose Answer
<36>A woman with glucose-6-phosphate dehydrogenase (G6PD) deficiency develops a urinary tract infection. Free radicals generated by responding neutrophils create an oxidant stress, and RBCs are rapidly overwhelmed. As soon as intravascular hemolysis begins, serum levels of which of the following will decrease? A. Bilirubin B. C-reactive protein C. Free iron D. Haptoglobin E. Methemoglobin Answer
<37>An urban health department reports the infant mortality rate of the city in the past year. This value corresponds to which of the following? A. The number of deaths during the past year from all causes divided by the total population B. The number of deaths occurring after the first 4 weeks of life and before the first birthday divided by the total number of live births C. The number of deaths occurring until the first birthday divided by the total number of live births D. The number of deaths occurring within the first 4 weeks of life divided by the total number of births E. The number of deaths occurring within the first 4 weeks of life divided by the total number of live births Answer
<38>A male infant presents with flattened facial features, low set ears , and deformities of the feet. The lungs are underdeveloped. The pregnancy was complicated by severe oligohydramnios. The most likely cause of this condition is a malformation of the A. paramesonephric ducts B. pronephros C. ureteric buds D. urogenital sinus E. urorectal septum Answer
<39>A 29-year-old female comes to her physician's office complaining of headaches, fatigue, and weakness over the past several months. Physical exam is significant for pallor, tachycardia, dizziness on standing up, and koilonychia (spooning of the nails). Laboratory studies show: Hemoglobin-10.2 g/dl Hematocrit-30.8 % Serum Fe-24 mg/dl Serum ferritin-30 ng/ml Total Fe binding capacity-713 mg/dl A peripheral blood smear would likely show A. macrocytosis with hypersegmented neutrophils B. microcytosis with basophilic stippling C. microcytosis with hypochromia D. numerous schistocytes Answer
<40>A 3-year-old boy presents with a 1-day history of loose stools, fever, abdominal cramping, headache, and myalgia. He has no blood in the stool. A careful history reveals that he has several pet turtles. Which of the following is most likely the causative agent of his diarrhea? A. Chlamydia psittaci B. Entamoeba histolytica C. Salmonella spp. D. Staphylococcus aureus E. Yersinia enterocolitica Answer
<41>A newborn baby has a large, cystic "mass" of the lumbar region. The mass is found to consist of CSF-filled meningeal tissue that has herniated through a vertebral defect. The child moves all her extremities and responds to external stimulation in a normal fashion. The term best used to describe this child's lesion is which of the following? A. Encephalocele B. Meningocele C. Meningomyelocele D. Spina bifida aperta E. Spina bifida occulta Answer
<42>A medical student, whose baseline alveolar PCO2 level was 40 mm Hg, begins to voluntarily hyperventilate for an experiment during his respiratory physiology laboratory. If his alveolar ventilation quadruples and his CO2 production remains constant, approximately what will be his alveolar PCO2? A. 4 mm Hg B. 10 mm Hg C. 20 mm Hg D. 80 mm Hg E. 160 mm Hg Answer
<43>A 32-year-old woman visits her gynecologist for a Pap smear. On physical examination, her gynecologist palpates a large adnexal mass on the right. After ultrasound confirmation of a large ovarian mass, a laparotomy is scheduled, and the mass is removed. Pathologic examination of the mass demonstrates a cystic cavity filled with hair and keratin debris, and the wall contains skin, adnexal tissue, thyroid tissue, and neural tissue. All of the tissues are similar to those normally found, and no malignant changes are seen. Which of the following is the most likely diagnosis? A. Immature teratoma B. Leiomyoma C. Leiomyosarcoma D. Mature teratoma E. Rhabdomyosarcoma Answer
<44>An 82-year-old woman with congestive heart failure and a creatinine clearance (CrCl) of 17 mL/min needs a diuretic for treatment of peripheral edema. Which of the following diuretics would be most appropriate in this patient? A. Furosemide B. Hydrochlorothiazide C. Indapamide D. Spironolactone E. Triamterene Answer
<45>A hypertensive patient is found to have a partial obstruction of the renal artery due to an atherosclerotic plaque. The resultant decrease in blood flow causes the increased release of an enzyme from which of the following structures? A. Afferent arterioles B. Arcuate arteries C. Juxtaglomerular cells D. Kupffer cells E. Proximal convoluted tubule Answer
<46>A Native American man is brought to a rural hospital in New Mexico. On arrival, he is unconscious with severe bronchopneumonia. Family members state that he suffered the sudden onset of chills, fever, and headache several days ago. One day later, the man complained of chest pain and difficulty breathing, and coughed up blood-tinged sputum. Chest x-ray reveals patchy infiltrates and segmental consolidation. Which of the following organisms is the most likely cause of this man's pneumonia? A. Brucella abortus B. Clostridium perfringens C. Francisella tularensis D. Listeria monocytogenes E. Yersinia pestis Answer
<47>A 34-year-old woman complains of early morning awakenings and loss of interest in everyday activities. She is diagnosed with major depressive disorder and given fluoxetine, but does not improve. Tricyclic antidepressants and MAO inhibitors are subsequently tried without effect, and electroconvulsive therapy (ECT) is recommended.Which of the following represents the most serious side effect of ECT? A. Extrapyramidal symptoms B. Hearing loss C. Mania D. Retrograde amnesia E. Rhabdomyolysis Answer
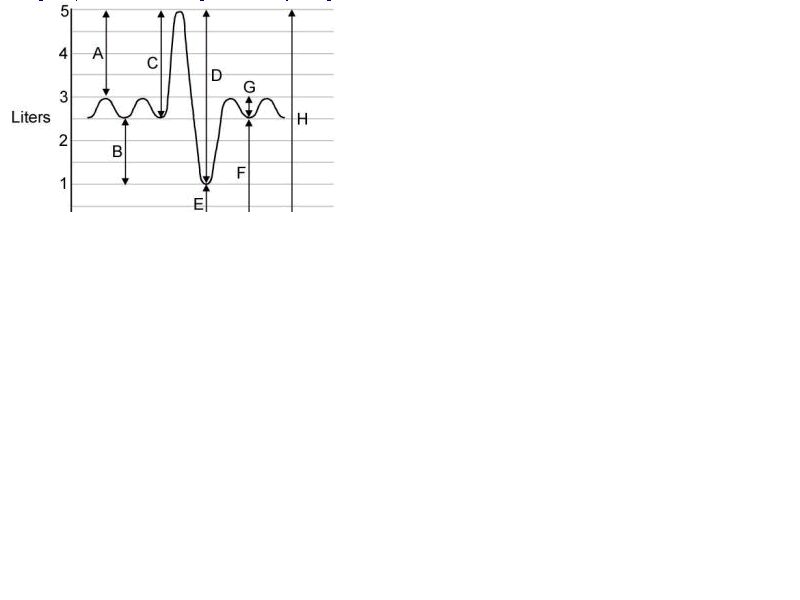
<48>A 62-year-old man with a 50-year-history of cigarette smoking has a complete work-up in a pulmonary function laboratory. The table below shows pulmonary volumes and capacities obtained using simple spirometry and helium washout techniques. Lung Volumes Values Functional residual capacity 5.0 L Inspiratory reserve volume 1.5 L Inspiratory reserve capacity 2.0 L Vital capacity 3.5 L What is the total lung capacity of this patient? A. 6.5 L B. 7.0 L C. 7.5 L D. 8.0 L E. 8.5 L Answer
<49>A patient arrives in the emergency room after having been stabbed. He has suffered a penetrating wound in the left fourth intercostal space immediately lateral to the sternal border. Which of the following thoracic structures is most likely to have been injured? A. Left atrium B. Left ventricle C. Right atrium D. Right ventricle E. Upper lobe of the left lung Answer
<50>A 60-year-old male presents to the dermatologist with a complaint o f tender blisters on his arm and flank. Physical examination reveals blisters and flaccid bullae; a few have ruptured, leaving red, sore, denuded areas. Which of the following findings would suggest the diagnosis of pemphigus vulgaris as opposed to bullous pemphigoid? A. Eosinophils within bullae B. IgA deposits on basement membrane C. IgG autoantibody activity D. Negative Nikolsky sign E. Oral mucosal lesions Answer
Answers
1The correct answer is A. The lesion is a squamous cell carcinoma of the skin. Actinic keratosis, which is a hyperplastic lesion of sun-damaged skin, predisposes for squamous cell carcinoma. Another predisposing condition to remember is xeroderma pigmentosum, which predisposes for both squamous cell and basal cell carcinomas of skin. A nevus is a mole, containing characteristic cells called nevocellular cells. If the nevocellular cells are located at the dermal-epidermal junction (junctional nevus, choice D), in the dermis (dermal nevus, choice C), or both (compound nevus, choice B), they do not predispose for squamous cell carcinomas of the skin. Malignant melanoma (choice E), however, can arise in pre-existing nevi.
2The correct answer is C. In renal failure, the ability of the kidney to secrete phosphate is impaired. The resultant hyperphosphatemia causes hypocalcemia and triggers excretion of large amounts of parathyroid hormone. The released parathyroid hormone is a major contributor to bony changes (e.g., osteitis fibrosa, a form of localized bone resorption) seen in some patients with chronic renal failure. Aldosterone (choice A) is a regulator of serum sodium. Calcitonin (choice B) levels are usually low in chronic renal failure, unless the parathyroids have so hypertrophied as to cause "tertiary hyperparathyroidism" with hypercalcemia. Renin (choice D) is normally secreted by the kidney and may be either decreased or increased in varying stages and forms of kidney disease. Regardless, renin regulates blood pressure and aldosterone secretion, rather than bone metabolism. The active form of Vitamin D (choice E), cholecalciferol, is formed in the kidney from Vitamin D absorbed from the gut and then processed by the liver. Uremia interrupts this pathway and consequently causes a functional Vitamin D
3The correct answer is C. Lysozyme is present in tears, saliva, mucus, vaginal secretions, and several other body fluids. This material lyses the peptidoglycan layer of the cell wall of bacteria without participation of any of the elements of the oxidative killing pathway. Hydrogen peroxide (choice A) is formed in the oxidative killing pathway from the superoxide ions. This material is also very toxic to bacteria pathogens. Hypochlorous acid (choice B) is formed from hydrogen peroxide and halide ions in the presence of myeloperoxidase. Myeloperoxidase (choice D) is an enzyme present in the oxidative killing pathway that breaks down hydrogen peroxide. Superoxide ions (choice E) are formed by NADPH oxidase in the first reaction of the oxidative killing pathway. These superoxide ions are extremely toxic to bacterial organisms.
4The correct answer is E. Secobarbital is a short-acting barbiturate with considerable dependence potential. Withdrawal from short-acting barbiturates can produce anxiety, delirium, and seizures which may be accompanied by life-threatening cardiovascular collapse. Insomnia (choice A) is a complication of barbiturate withdrawal, since barbiturates are sedative/hypnotic agents, but this complication is not serious enough to be a contraindication to abrupt cessation of the drug. Rebound anxiety (choice B) would be quite likely following abrupt cessation of the barbiturate, but would not constitute a sufficient danger to the patient to preclude self-detoxification. Recidivism (choice C) is quite likely in drug abusers, with or without medical intervention. Respiratory depression (choice D) is common with acute administration of barbiturates, but would not be expected with barbiturate abstinence.
5The correct answer is A. The baby has meconium ileus, which is a manifestation of cystic fibrosis due to the abnormally viscid pancreatic secretions which "get stuck" in the small bowel. Meconium ileus can cause gut perforation with peritonitis and intraperitoneal calcifications (that may be visible on plain film). Meconium ileus complicated by intestinal perforation or formation of fistulas to the bladder or vagina must be treated surgically. Medical treatments for uncomplicated meconium ileus are now available, which use enemas, mucolytic agents, or pancreatic enzymes. Hirschsprung's disease (choice B) is a cause of congenital constipation related to absence of ganglion cells in a segment of bowel. The aganglionic bowel segment is narrowed because the lack of peristalsis keeps stool from moving into the segment. The distal rectum is always involved, and the lesion may extend proximally as far as the small intestine. The bowel proximal to the lesion is usually dilated. A Meckel's diverticulum (choice C) can form due to the persistence of the vitelline duct, which connects the developing gut to the yolk sac. They are classically located in the distal ileum within 30 cm of the ileocecal valve, and may contain ectopic pancreatic tissue or gastric mucosa.
6The correct answer is E. Misoprostol, a methyl analog of prostaglandin E1, is approved for the prevention of ulcers caused by the administration of nonsteroidal anti-inflammatory agents. Because this drug is a potential abortifacient, it should not be given to pregnant women, or to women who are attempting to conceive. Antinuclear antibodies (choice A) are associated with autoimmune diseases such as systemic lupus erythematosus, scleroderma, Sj�gren's syndrome, and inflammatory myopathies. The test would be of no value in this case. A barium swallow (choice B) is not indicated prior to the administration of misoprostol. Esophageal manometry (choice C) is used to evaluate the competency of the lower esophageal sphincter, and to assess esophageal motor activity. The osmotic fragility test (choice D) is performed by placing erythrocytes into a low-salt solution. An increased susceptibility to osmotic lysis is found in hereditary spherocytosis.
7The correct answer is B. Inversion of the heart, so that the morphologic left ventricle is in the right chest, is called dextrocardia. Isolated dextrocardia is almost always associated with cardiac defects that may include transposition of the atria and transposition of the great arteries. However, dextrocardia as part of situs inversus totalis, with reversal of the thoracic and abdominal organs, is usually associated with a physiologically normal heart. The cluster of situs inversus, sinusitis, and bronchiectasis is called Kartagener syndrome, which is caused by defective ciliary function. Since migration of some embryonic cells during development appears to be dependent on ciliary function, this is thought to explain the situs inversus. You should associate Down syndrome (choice A) with an ostium primum type of atrial septal defect. You should associate Kawasaki disease (choice C) with coronary artery aneurysms. You should associate Marfan syndrome (choice D) with aortic dissection. You should associate Turner syndrome (choice E) with coarctation of the aorta.
8The correct answer is C. The lesion is commonly called a Baker's cyst, and anatomically represents an enlarged semimembranous bursa. Baker's cysts are more commonly seen at the extremes of age. The deep infrapatellar bursa (choice A) is on the anterior aspect below the knee. The prepatellar bursa (choice B) is anterior to the patella. The superficial infrapatellar bursa (choice D) is on the anterior aspect of the leg below the knee. The suprapatellar bursa (choice E) is on the anterior aspect of the thigh above the knee.
9The correct answer is E. The esophagus is covered by non-keratinized, stratified, squamous epithelium for its entire length. Heartburn is usually a sign of gastric regurgitation of the acidic contents in the lower esophagus (acid reflux disease). Acid reflux disease is a serious problem that may be associated with a precancerous condition (Barrett's esophagus).
10The correct answer is C. This man has received repetitive trauma to his right arm from operating a jack hammer for long periods of time. The median nerve is affected, as evidenced by decreased sensation in its distribution (first three-and-a-half). Thus, the muscles in the hand innervated by the median nerve will likely also be affected, such as the thenar muscles (abductor pollicis brevis, opponens pollicis, and flexor pollicis brevis) and the first two lumbricals. All other intrinsic muscles of the hand are innervated by the ulnar nerve (abductor digiti minimi, dorsal interossei, choices A and B). The wrist extensors (choice D) are innervated by the radial nerve and the supinators (choice E) are innervated as follows: biceps brachii-musculocutaneous nerve, supinator-radial nerve, brachioradialis-radial nerve.
11The correct answer is C. Nephroblastoma (Wilms tumor) characteristically affects children between 2 and 4 years of age and can form large spherical masses composed of variegated tissues including primitive renal epithelial elements, a sarcomatous-appearing stroma, abortive glomeruli and tubules, and heterologous tissues such as muscle, cartilage, fat, and bone. Cortical adenoma (choice A) is a small (under 2 cm) benign tumor that is usually found incidentally at autopsy. Hemangiomas (choice B) can occur in the kidney, but would not usually produce a large mass. Oncocytomas (choice D) are benign tumors that can be large but do not usually affect young children. Renal cell carcinoma (choice E) is usually a disease of older adults.
12The correct answer is E. The facial nerve (CN VII) is intimately related anatomically to the parotid gland, but controls salivation from both the submandibular and sublingual glands. The parotid gland (choices A, B, and C) is innervated by the glossopharyngeal nerve (CN IX).
13The correct answer is A. Burkitt's lymphoma is actually associated with three translocations. The common variant t(8;14)(q24;q32), involving the oncogene myc on chromosome 8, and the heavy immunoglobulin chain on chromosome 14. The other two variants are: t(8;22)(q24;q11), involving myc and the lambda light chain immunoglobulin site, and t(2;8)(p12;q24), involving the kappa light chain and myc. Mantle cell lymphoma (choice B), multiple myeloma (choice C), and small (not cleaved) cell lymphoma (choice D) are associated with the t(11;14)(q13;q32) translocation involving bcl -1 and the heavy chain site. Small cleaved cell lymphoma (choice E) is associated with t(14;18)(q 32;q21), involving the immunoglobulin chain site and bcl-2.
14The correct answer is C. The defecation reflex that is evoked when the rectum is distended involves three responses: 1) the internal anal sphincter relaxes, 2) the external anal sphincter contracts, and 3) a conscious urge to defecate is perceived. This neural reflex involves the pelvic nerve, which provides the parasympathetic preganglionic innervation to the internal anal sphincter (composed of smooth muscle) and also carries the sensory afferent information from the rectum to the spinal cord, and the pudendal nerve, which carries the somatic efferent inputs to the external anal sphincter (composed of skeletal muscle). In the patient described above, the pelvic nerve is most likely damaged since neither the reflex relaxation of the internal anal sphincter nor the urge to defecate is evoked by rectal distention. Damage to the internal anal sphincter (choice A) would most likely cause resting tone to be low and, if anything, lead to fecal incontinence rather than constipation. Furthermore, damage to the internal anal sphincter could not explain the failure of the appearance of the urge to defecate. The external anal sphincter (choice B) appears to function normally since distention of the rectum evokes the expected contraction. The normal contraction of the external anal sphincter also suggests that the pudendal nerve (choice D) is intact. Since distention of the rectum (choice E) evoked the contraction of the external anal sphincter, it too appears to be functioning normally.
15The correct answer is A. The spots described are called Roth's spots, and specifically suggest bacterial endocarditis. They represent small fibrin clots that form on the vegetations and then break off and lodge in small blood vessels, including those of the retina. Splinter hemorrhages, petechiae, and small, painful nodules on the finger and toe pads (Osler's nodes) may also be seen. Physical examination frequently reveals a heart murmur. Crohn's disease (choice B) can occasionally be associated with uveitis, but not retinal hemorrhages. Diabetes mellitus (choice C) can cause a variety of ocular changes including microaneurysms, flame hemorrhages, and "cotton wool" deposits, but Roth's spots are not produced. Glaucoma (choice D) causes increased pressure in the anterior chamber, but does not produce Roth's spots. Urosepsis (choice E) does not usually cause any obvious eye findings.
16The correct answer is E. The patient is suffering from mitral regurgitation caused by rupture of the chordae tendineae. Mitral regurgitation is characterized by a greatly elevated left atrial pressure toward the end of systole caused by backward flow of blood from the left ventricle into the left atrium through the leaky mitral valve. The left atrial pressure is normal at the end of diastole with mitral regurgitation because blood flows unimpeded from the atrium into the ventricle when the mitral valve is open. The leak occurs during systole, and is characterized by a systolic murmur, which was noted in the patient. The chordae tendineae are tendinous cords that connect each cusp of the mitral valve to the papillary muscles in the left ventricle. When these rupture, the cusps of the mitral valve cannot be approximated during systole, which results in backward flow of blood into the left atrium. The chordae tendineae are often damaged in rheumatic valvular disease, which increases the probability of rupture. The aortic pressure and left ventricular pressure tracings are nearly superimposed during systole in the diagram, which eliminates the possibility of aortic obstruction (choice A) and aortic regurgitation (choice B). The rate of rise of left ventricular pressure appears to be normal, which argues against the possibility of left ventricular infarction (choice C). In mitral obstruction (choice D), the left atrial pressure is greater than the left ventricular pressure toward the end of diastole when blood is flowing from the left atrium into the left ventricle.
17The correct answer is E. This is the classic presentation of Zenker's diverticulum, which is a false diverticulum formed by herniation of the mucosa at a point of weakness at the junction of the pharynx and esophagus in the posterior hypopharyngeal wall. Zenker's diverticulum is also associated with halitosis, and if the diverticulum fills completely with food, it can cause dysphagia or obstruction of the esophagus. Mallory-Weiss tears (choice A) are mucosal tears at the gastroesophageal junction secondary to repeated, forceful vomiting. They are often seen in alcoholics. Plummer-Vinson syndrome (choice B) is the triad of dysphagia (due to esophageal webs in the upper esophagus), atrophic glossitis, and iron-deficiency anemia. Schatzki rings (choice C) are mucosal rings found in the distal esophagus at the squamocolumnar junction. In contrast to a Zenker's diverticulum, the usually asymptomatic traction diverticula (choice D) are true diverticula involving all of the layers of the esophagus. They are typically caused by adherence of the esophagus to a scarred mediastinal structure.
18The correct answer is B. In obstructive lung disease such as emphysema, the MEFV curve begins and ends at abnormally high lung volumes, and the flow rates are lower than normal at any given lung volume. Note on the diagram that the patient's total lung capacity is 7 liters and the residual volume is 3.5 liters (dashed curve). The curve may also have a scooped out appearance as shown on the diagram. Note that absolute lung volumes cannot be determined from a MEFV curve alone. An additional method is used to measure residual volume, then the curves can be placed appropriately on the abscissa. Lung volumes are expected to be lower than normal in asbestosis (choice A), pleural effusion (choice C), pneumothorax (choice D), silicosis (choice E), and other types of restrictive lung diseases.
19The correct answer is B. In the formation of the upper lip, the right and left medial nasal prominences merge to form the philtrum of the upper lip. The lateral maxillary prominence then merges with the merged medial nasal prominences. Failure of this merger to occur results in a unilateral cleft lip. Failure of a lateral palatine process to fuse with the median palatine process (choice A), which is synonymous with a failure of the primary palate to fuse with the secondary palate (choice C), results in a primary cleft palate. Primary clefts of the palate are found anterior to the incisive foramen of the palate. Primary cleft palates may occur along with cleft lips but are the result of a separate developmental defect. Failure of the right and left medial nasal prominences to merge (choice D) results in a median cleft lip. This is a rare anomaly. Normally, the right and left medial nasal prominences merge into a single prominence which forms the philtrum of the lip. Failure of the right and left palatine processes to fuse (choice E) results in a secondary cleft palate. Secondary cleft palates are found posterior to the incisive foramen. Normally, the right and left palatine processes fuse together and fuse to the primary palate.
20The correct answer is B. Disseminated intravascular coagulation (DIC) is characterized by consumption of both platelets and clotting factors. The best tests to order are platelet count (which will be markedly decreased), serum fibrinogen level (which will be low), and fibrin degradation products (which will be high). Prothrombin time (PT) measures factors I (fibrinogen), II, V, VIII, and X. Partial thromboplastin time (PTT) measures VII, prekallikrein, high-molecular weight kininogen, and factors I, II, V, VII, IX, X, and XI. Both PT and PTT are relatively non-specific. Thrombin time (TT) is a more specific measure of fibrinogen and would potentially be a useful test in this setting. However, specific measurement of factor VIII, kininogen, or prekallikrein levels would not be rational in evaluating DIC.
21The correct answer is A. This is Addison disease, in which severe adrenal disease produces adrenocortical insufficiency. Causes include autoimmune destruction, congenital adrenal hyperplasia, hemorrhagic necrosis, and replacement of the glands by either tumor (usually metastatic) or granulomatous disease (usually tuberculosis). The symptoms can be subtle and nonspecific (such as those illustrated), so a high clinical index of suspicion is warranted. Skin hyperpigmentation is a specific clue that may be present on physical examination, suggesting excess pituitary ACTH secretion. (The ACTH precursor has an amino acid sequence similar to MSH, melanocyte stimulating hormone.) Most patients have symptoms (fatigue, gastrointestinal distress) related principally to glucocorticoid deficiency. In some cases, however, mineralocorticoid replacement may also be needed for symptoms of salt wasting with lower circulating volume. Except in the case of primary pancreatic cancer, complete tumor replacement of the endocrine pancreas (choice B) would be uncommon. In any event, pancreatic involvement would be associated with diabetes mellitus. Involvement of the ovaries (choice C) by metastatic tumor (classically gastric adenocarcinoma) would produce failure of menstruation. Involvement of the pituitary gland (choice D) could produce Addisonian symptoms, but the pigmented skin suggests a primary adrenal problem rather than pituitary involvement. Replacement of the thyroid gland (choice E) by tumor would cause hypothyroidism with lesser degrees of fatigue and cold intolerance; this is an unusual cause of hypothyroidism and is less likely to be tested than Addison disease caused by bilateral adrenal metastasis.
22The correct answer is B. When patients present with either a muscle spasm or a "strained" muscle, a centrally acting skeletal muscle relaxant is typically prescribed. In addition to these agents, a nonsteroidal anti-inflammatory drug is often added for additional pain control. Although somnolence can be seen with any of the agents listed, xerostomia (dry mouth), mydriasis and tachycardia are classic anticholinergic side effects. Cyclobenzaprine is a centrally acting skeletal muscle relaxant that is structurally related to tricyclic antidepressants, which are known for their strong anticholinergic side effects. Additional common anticholinergic side effects seen with this agent include blurred vision, urinary retention, and constipation. Less common side effects include agitation, respiratory depression, disorientation, tachycardia, and widening of the QRS complex. Baclofen (choice A) is a centrally acting skeletal muscle relaxant that produces muscle relaxation by inhibition of both monosynaptic and polysynaptic reflexes at the spinal level. This agent is indicated for the treatment of spasticity resulting from multiple sclerosis or secondary to spinal cord injuries; it has also been used in the treatment of trigeminal neuralgia. The most common side effects include transient drowsiness, fatigue, and hypotension. Diclofenac (choice C) is a non-steroidal anti-inflammatory drug indicated for the treatment of a variety of disorders associated with pain and inflammation. The most common side effects include dyspepsia, nausea, vomiting, abdominal cramps, and dizziness. Methocarbamol (choice D) produces muscle relaxation by general CNS depression; it does not have a direct action on the contractile mechanism of striated muscle or nerve fibers. This agent is indicated as an adjunct to rest, physical therapy, and other measures for relief of discomfort in various musculoskeletal conditions. Reported side-effects include dizziness, vertigo, ataxia, headache, irritability, bradycardia, hypotension, and syncope. Rofecoxib (choice E) is a selective cyclooxygenase-2 (COX-2) inhibitor with anti-inflammatory, analgesic, and antipyretic effects. This agent is used in adults for relief of pain and inflammation caused by osteoarthritis and rheumatoid arthritis, as well other inflammatory conditions. The most common side effects are nausea, vomiting, diarrhea, abdominal distress, flatulence, and anorexia.
23The correct answer is A. The patient has Dressler's syndrome, which is thought to be an autoimmune phenomenon resulting in fibrinous pericarditis with fever and pleuropericardial chest pain several weeks after a myocardial infarction. Bacterial (choice B), fungal (choice D), and viral (choice E) infections can cause pericarditis, but would not be suspected in the setting of myocardial infarction. Chlamydia (choice C) are not a usual cause of pericarditis.
24The correct answer is B. The lesion described is the form of in situ penile carcinoma known as Bowen's disease. Bowen's disease is thought to carry a 10% risk of progressing to invasive squamous cell carcinoma, if left untreated. Bowenoid papulosis (choice A) is a form of in situ penile carcinoma that is characterized clinically by multiple, reddish-brown, papular lesions. Condyloma acuminatum (choice C) is a benign lesion that resembles the common wart. Condylomata are associated with papillomavirus infection. Erythroplasia of Queyrat (choice D) is a form of in situ penile carcinoma that produces a soft, red plaque. Giant condyloma (choice E) is an uncommon variant of condyloma acuminatum that is locally aggressive, but does not usually metastasize.
25The correct answer is C. Acute epididymitis and orchitis with prominent neutrophils in a sexually active male are most likely due to infection with Neisseria gonorrhoeae or Chlamydia trachomatis. N. gonorrhoeae can produce a nonspecific pattern of acute inflammation (nonspecific epididymitis and orchitis) or can be sufficiently severe as to cause frank abscesses within the epididymis. Escherichia coli (choice A) is an important cause of nonspecific epididymitis and orchitis in children with congenital genitourinary abnormalities and in older men. Mycobacterium tuberculosis (choice B) can cause tuberculosis of the epididymis and testes, characterized by granuloma formation. Pseudomonas sp.(choice D) has been implicated as an important cause of nonspecific epididymitis and orchitis in older men. Treponema pallidum (choice E), the causative agent of syphilis, can cause testicular involvement with gumma formation, endarteritis, and/or a prominent plasma cell infiltrate.
26The correct answer is C. The cardiac output (CO) is equal to the volume of blood ejected from the heart during each systole (i.e., the stroke volume; SV) multiplied by the number of times the heart beats each minute (heart rate; HR). In other words, CO = SV x HR. Therefore, SV = CO/HR, and since CO = 5000 mL/min, and HR = 50/min, SV = 5000/50 = 100 mL.
27The correct answer is A. Even if you do not remember the features of the individual lipid storage diseases, it is worth remembering that Fabry's disease (described above) is the only one in the group with X-linked genetics. As a general rule, you should associate all of the lipid storage diseases with severe neurologic deterioration. The exception is Gaucher's disease (choice B), which tends to affect the liver and spares the brain. Gaucher's disease (choice B), Niemann-Pick disease (choice E), and Type I Tay-Sachs disease are not X-linked; all occur with greater frequency in Ashkenazi Jews. You should associate Krabbe's disease (choice C) with the presence of "globoid" cells in degenerating white matter in the brain. Metachromatic leukodystrophy (choice D) is caused by a deficiency of the enzyme arylsulfatase A.
28The correct answer is B. This is Bowen's disease, which is one clinical form of penile carcinoma in situ (the other forms are Bowenoid papulosis and erythroplasia of Queyrat). Untreated Bowen's disease will, over a period of years, progress to frank invasive carcinoma in 10% to 20% of patients. Bowen's disease can affect the genital region of both men and women. Bowenoid papulosis (choice A) is another form of penile carcinoma in situ, characterized clinically by multiple reddish-brown papular lesions. Condyloma acuminatum (choice C) usually produces a papillary lesion. Erythroplasia of Queyrat (choice D) is another form of penile carcinoma in situ, characterized by single or multiple shiny red plaques. Squamous cell carcinoma (choice E) will be frankly invasive on biopsy.
29The correct answer is C. In young women, the most likely causes of cervicitis and pelvic inflammatory disease (PID) are Neisseria gonorrhoeae and Chlamydia trachomatis. Gram's staining alone may not be able to distinguish between the two in women, so culture is warranted. Both organisms induce endocytosis by epithelial cells. Neisseria gonorrhoeae is a gram-negative diplococcus. It is endocytosed by mucus-secreting epithelia, and is exocytosed into subepithelial tissues leading to necrotizing acute inflammation and destruction of ciliated and non-ciliated cells. Through direct extension, it can lead to PID and infertility in women. It can be detected by visualizing the organism in polymorphonuclear leukocytes (PMNs) in Gram's stained clinical material more easily in men than in women. Therefore, culture onto Thayer-Martin agar is usually required for diagnosis in women. Since the organism can be cultured, it is not an obligate intracellular parasite (compare with choice D). The organism can be killed by PMNs, antibody, and complement, however, many of its outer membrane proteins undergo antigenic or phase variation or cause the production of blocking antibody that interferes with bactericidal activity. Immunity to the organism does not develop (compare with choices A and B). Neisseria gonorrhoeae is resistant to penicillin, a b-lactam antibiotic (compare to choice E), because of a plasmid-mediated penicillinase and a chromosomally-mediated mutation that decreases the permeability of the outer membrane and decreases the affinity of penicillin binding proteins. It can be treated with ceftriaxone, a cephalosporin, which resists the penicillinase, or with quinolones and azithromycin. Chlamydia trachomatis is an obligate intracellular parasite (choice D) that induces endocytosis and resides in the phagosome of infected epithelial cells. It possesses a gram-negative envelope but lacks peptidoglycan, and hence is intrinsically resistant to all antibiotics that inhibit peptidoglycan synthesis, such as the b-lactam antibiotics (compare with choice E). Antibodies are ineffective at controlling infection. Cell mediated immunity (choice A) is probably the major means of controlling this infection since a deficiency in cell mediated immunity both increases susceptibility and severity in animal models. Chronic and clinically latent infections cause serious morbidity, including pelvic inflammatory disease, fallopian tube dysfunction and blindness. Chlamydia infection can be treated with macrolides, quinolones and tetracyclines.
30The correct answer is C. Methotrexate is a type of disease-modifying antirheumatic drug (DMARD). DMARDs are a varied group of drugs, including methotrexate, azathioprine, penicillamine, hydroxychloroquine and chloroquine, organic gold compounds, and sulfasalazine, which are thought to slow the progression of rheumatoid arthritis by modifying the disease itself. However, these drugs can take several weeks to several months to produce therapeutic effects. In rheumatoid arthritis, prednisone is used when persistent synovitis is seen in multiple joints despite sufficient dosage of NSAIDs. It is also used for "bridge" therapy when DMARD therapy with methotrexate is first initiated. Because it takes a long time for the therapeutic effect of DMARDs to become evident, agents like prednisone are needed to "bridge the gap" between NSAID therapy and DMARD therapy. The major disadvantage of using glucocorticoids for an extended period of time is the severe side effect profile. For example, long term use of prednisone is associated with hypocalcemia (choice C), fluid retention (not dehydration, choice A), hypokalemia (not hyperkalemia, choice B), hyperglycemia (not hypoglycemia, choice D), and hypernatremia (not hyponatremia, choice E). Other adverse reactions include adrenal suppression, muscle weakness and atrophy, gastritis, nausea, vomiting, Cushingoid state (moon face, buffalo hump, central obesity), immunosuppression, hypertension, psychosis, osteoporosis, glaucoma, and posterior subcapsular cataracts.
31The correct answer is A. The brachial artery is immediately medial to the tendon of the biceps brachii at the elbow. As the artery enters the forearm, it is covered by the bicipital aponeurosis, a broadening of the biceps tendon. The musculocutaneous nerve (choice B) does not cross the elbow. The musculocutaneous nerve gives off all of its muscular branches to muscles in the arm. The remainder of the nerve is then renamed the lateral cutaneous nerve of the forearm, which passes the elbow lateral to the tendon of the biceps. The profunda brachii artery (choice C) arises from the brachial artery in the proximal part of the arm. It accompanies the radial artery in the musculospiral groove and then divides into the radial collateral artery and middle collateral artery, which cross the elbow lateral to the tendon of the biceps. The radial nerve (choice D) lies within the musculospiral groove along the back of the humerus, then passes between the brachioradialis muscle and the brachialis muscle at the elbow, lateral to the tendon of the biceps. The ulnar nerve (choice E) crosses the elbow posterior to the medial epicondyle of the humerus. It then passes between the two heads of the flexor carpi ulnaris and courses through the forearm deep to this muscle.
32The correct answer is C. A thiazide diuretic would be the drug of choice for this patient because it is the only class of diuretic which decreases urinary secretion of calcium. Thiazide diuretics, like hydrochlorothiazide, inhibit the Na+/Cl- cotransporter in the distal convoluted tubule and promote the reabsorption of calcium. Acetazolamide (choice A), a carbonic anhydrase inhibitor, and furosemide (choice B), a loop diuretic, both induce diuresis at the expense of all three major cationic electrolytes (Na+, K+, and Ca2+) which are secreted in increased amounts. Spironolactone (choice D) and triamterene (choice E), so-called potassium sparing diuretics, block Na+/K+ exchange in the collecting duct. Although they decrease K+ secretion, Na+ and Ca2+ secretion are elevated.
33The correct answer is D. The patient's initial hyperlucent lung fields strongly suggest the presence of emphysema. The radiologic findings after the increase in shortness of breath are consistent with free air in the chest, which has collapsed the left lung and caused a shift in the location of the mediastinum. Such air might have been introduced by rupture of a bulla. Small pneumothoraces are usually well tolerated, but larger ones may require decompression (the needle from a syringe is sometimes used), or even surgical correction if bullae continue to leak air. Bronchogenic carcinoma (choice A) would be expected to produce a mass lesion. Pleural effusion (choice B) usually develops slowly, and causes a whitening of lung fields when fluid is present. Pulmonary embolism (choice C) can cause a sudden shortness of breath, but would not cause an increase in the lucency of the lung fields. Tuberculosis (choice E) would be expected to produce a mass lesion in the lung
34The correct answer is D. Therapy of diabetic ketoacidosis requires more than insulin. Intravascular volume is often depleted, and initial fluids to restore volume should include isotonic saline or lactated Ringer's solution. If arterial blood pH is less than 7.1 or if severe hyperkalemia is present, bicarbonate supplementation should be used. IV fluids containing 5-10% dextrose (glucose) should be used when the serum glucose levels fall to 200-300 mg/dL, since high doses of rapidly acting insulin can cause life-threatening hypoglycemia. Additionally, the serum potassium concentration should be watched very carefully, since potassium is cotransported into cells with glucose in the presence of insulin. It is often the case that hyperkalemia is present initially, secondary to decreased cellular uptake of potassium with decreased cellular uptake of glucose. However, this can rapidly change when insulin drives glucose (with potassium) into cells, and a life-threatening hypokalemia can develop. Supplementation with calcium (choice A) is not required with insulin administration. Creatinine (choice B) is a waste product, rather than a nutrient. Supplementation with magnesium (choice C) is not required with insulin administration. Sodium supplementation (choice E) is not required during therapy with insulin.
35The correct answer is D. The amount of glycosylated hemoglobin (HbA1c) is directly related to the level of glucose in the blood. Since HbA1c is a stable product, its concentration reflects glucose levels over the past 3-6 months. HbA1c forms as a result of nonenzymatic glycosylation, a fundamental biochemical abnormality that accounts for most of the histopathologic alterations in diabetes mellitus. At first, glucose forms reversible glycosylation products with proteins by formation of Schiff bases. Rearrangement of Schiff bases leads to more stable, but still reversible, Amadori products and subsequently to irreversible advanced glycosylation end products (AGE), of which HbA1c is an example. Blood ketones, blood glucose, urinary glucose, and blood insulin do not reflect long-standing metabolic abnormalities of diabetes mellitus and cannot be used to assess long-term glycemic control. Blood glucose (choice A) is elevated in both type 1 and type 2 diabetes mellitus. Hyperglycemia is the diagnostic feature of diabetes mellitus and leads to glycosuria (choice E) when blood glucose exceeds 160-180 mg/dL. Blood insulin (choice B) is decreased in untreated type 1 diabetes and normal or even slightly increased in type 2 diabetes. Blood ketones (choice C) (acetoacetic acid and b-hydroxybutyric acid) are synthesized from free fatty acids in response to severe insulin deficiency. Accumulation of ketone bodies in the blood is a crucial pathogenetic factor in ketoacidosis, which occurs exclusively in type 1 diabetics.
36The correct answer is D. Haptoglobin (or alpha-2 globulin) is a serum protein that promptly binds to free hemoglobin in the serum, forming a tight complex. The haptoglobin-hemoglobin complex is quickly cleared from the blood by the reticuloendothelial system, which allows the hemoglobin to be salvaged instead of lost into the urine. Intravascular hemolysis from any cause is rapidly followed by a dramatic drop in serum haptoglobin. Bilirubin (choice A) is synthesized in the liver and spleen as an end-product of heme degradation. Serum bilirubin levels would not change until the haptoglobin in the blood was completely saturated, and free hemoglobin began to circulate. In this circumstance, serum bilirubin would increase, not decrease. C-reactive protein (choice B) is an acute phase reactant produced by the liver in increased quantity in response to inflammation. This patient's urinary tract infection would increase C-reactive protein levels, but the hemolysis would not further affect them. Serum free iron (choice C) does not change appreciably in intravascular hemolysis. Ferrous iron in the red blood cell is complexed to hemoglobin, and this complex is not broken in hemolysis. Methemoglobin (an oxidized form of hemoglobin; choice E) increases in the blood along with free hemoglobin in cases of intravascular hemolysis.
37The correct answer is C. This is one of those questions where predicting the correct answer will facilitate your selecting the appropriate answer choice. Make sure to read each choice carefully (for example, choices D and E, though both incorrect in this case, look almost identical and could cost you points if you were not reading actively). Choice A refers to the crude mortality rate. Choice B refers to the postnatal mortality rate. Choice D is an incorrect rendering of the neonatal mortality rate since it considers the total number of births instead of the total number of live births. Choice E refers to the neonatal mortality rate.
38The correct answer is C. This infant suffers from Potter syndrome, caused by an absence of both kidneys. This is often caused by a failure of the ureteric buds to develop. The ureteric buds form the ureters, renal pelvis, calyces, and collecting tubules. The collecting tubules induce the formation of metanephric vesicles, which differentiate into the tubular components of the nephron. The paramesonephric ducts (choice A) form the uterine tubes, uterus, and the upper third of the vagina. The pronephros (choice B) is a transient collection of cells that disappears during the fourth week of development. It does not form the permanent kidney. The urogenital sinus (choice D) forms the urinary bladder (in both sexes). It also forms the prostatic urethra, prostate, membranous urethra, bulbourethral glands, penile urethra (proximal part) and Littre's glands in the male. In the female it forms most of the urethra, urethral glands, paraurethral glands, vestibule of the vagina and greater vestibular glands. The urorectal septum (choice E) partitions the cloaca into the urogenital sinus and rectum (and upper anal canal).
39The correct answer is C. This is a classic description of Fe deficiency anemia (up to 20% of adult women are Fe deficient!). Fe deficiency anemia is very common in menstruating women, and is associated with the signs and symptoms described (fatigue, weakness, pallor). It can also be associated with epithelial changes such as brittle nails and atrophic tongue. The typical laboratory values are those described along with a decreased reticulocyte count. On peripheral blood smear, the RBCs are small (microcytic) and pale in color (hypochromic, due to low Hb levels from inadequate Fe stores). Vitamin B12/folate deficiency would give you macrocytosis with hypersegmented neutrophils (choice A). Lead poisoning would give you microcytosis with basophilic stippling (choice B). Schistocytes (choice D) are RBC fragments seen when the cells are destroyed by shearing forces in the vascular system, such as those present in prosthetic heart valves and microangiopathic hemolytic anemias.
40The correct answer is C. Salmonella spp., including S. enteritidis and S. typhimurium, produce a gastroenteritis or enterocolitis. Patients with decreased gastric acidity, sickle cell disease, defects in immunity, or children younger than 4 years have a more severe course of disease. Salmonella spp. are carried in nature by animal reservoirs such as poultry, turtles, cattle, pigs, and sheep. The incubation period is 8-48 hours after ingestion of contaminated food or water. Chlamydia psittaci (choice A) produces an interstitial pneumonitis accompanied by headache, backache, and a dry, hacking cough. A pale, macular rash is also found on the trunk (Horder's spots). Patients at risk include pet shop workers, pigeon handlers, and poultry workers. Entamoeba histolytica (choice B) produces a diarrhea (frequently bloody or heme-positive), right lower quadrant crampy abdominal pain, and fever. Patients frequently have weight loss and anorexia. There is usually a history of travel outside the U.S. Most cases are chronic. Complications include liver abscesses. Staphylococcus aureus (choice D) produces a self-limited gastroenteritis due to the production of preformed, heat-stable enterotoxins. The incubation period is 16 hours. The toxins enhance intestinal peristalsis and induce vomiting by a direct effect on the CNS. Yersinia enterocolitica (choice E) usually produces a chronic enteritis in children. These patients have diarrhea, failure to thrive, hypoalbuminemia, and hypokalemia. Other findings include acute right lower quadrant abdominal pain, tenderness, nausea, and vomiting. The infection mimics appendicitis or Crohn's disease.
41The correct answer is B. Meningocele occurs due to a failure of closure of the caudal portion of the neural tube. In contrast to the more serious meningomyelocele, in which the spinal cord also herniates through the vertebral defect, meningocele is typically associated with only minimal neurological damage and is relatively easy to treat surgically. Encephalocele (choice A) implies herniation of the brain through a bony defect in the skull caused by defective closure of the cranial end of the neural tube. Meningomyelocele (choice C) includes herniation of the spinal cord through a vertebral defect. Associated neurological deficits are usually severe. In spina bifida aperta (choice D), there is a complete failure of fusion of the neural plate associated with malformation of the vertebral arches such that the underdeveloped neural plate is covered only with skin. No mass lesion is present, and the patient typically has major neurologic deficits. Spina bifida occulta (choice E) is the mildest of the neural tube defects, typically consisting of a small vertebral defect with a normal spinal cord and meninges. The defect is often associated with a skin dimple that overlies adipose tissue, hair follicles, or a sinus.
42The correct answer is B. When you hyperventilate, CO2 is blown off. The amount of CO2 blown off is inversely proportional to alveolar ventilation. This is shown by the alveolar ventilation equation: VA = VCO2/PACO2, where VA = alveolar ventilation VCO2 = CO2 production PACO2 = alveolar PCO2 So, if VCO2 remains the same, and VA quadruples, PACO2 must decrease by 4 fold; 40 mm Hg decreases to 10 mm Hg.
43The correct answer is D. The lesion is a mature teratoma. Teratomas located in the ovary and containing a hair and keratin filled cyst are sometimes called dermoid cysts. Teratomas contain cells of a variety of types, often including skin, skin adnexal structures (hair follicles, sweat glands, sebaceous glands), connective tissues, neural tissue, muscle, and thyroid tissue. If immature tissues such as primitive neuroepithelial cells or developing skeletal muscle cells are seen, the lesion is considered potentially malignant and classified as an immature teratoma (choice A). Leiomyomas (choice B) are benign tumors of smooth muscle (e.g., uterine "fibroids"), usually in the female genital tract. Leiomyosarcomas (choice C) are rare malignant tumors of smooth muscle, usually in the female genital tract. Rhabdomyosarcomas (choice E) are malignant skeletal muscle tumors with a predilection for the head and neck and urogenital regions in children.
44The correct answer is A. The key to this question is understanding that the effectiveness of each diuretic is dependent on the creatinine clearance (CrCl). For example, the "loop" diuretics are effective down to a CrCl of around 10 mL/min. However, the thiazide and potassium-sparing diuretics are effective only down to a CrCl of around 40 mL/min. Therefore, on the basis of this patient's CrCl of 17 mL/min, only a loop diuretic would be recommended. Furosemide is a loop diuretic that is indicated for the treatment of edema associated with congestive heart failure, hepatic cirrhosis, and renal disease. Hydrochlorothiazide (choice B) and indapamide (choice C) are thiazide diuretics and therefore would not be recommended for patients with such a low CrCl. Spironolactone (choice D) and triamterene (choice E) are potassium-sparing diuretics and therefore would not be recommended for a patient with a CrCl of 17 mL/min.
45The correct answer is C. The juxtaglomerular cells are in the wall of the afferent arteriole, close to the glomerulus. In response to decreased blood pressure, they secrete renin, an enzyme that converts angiotensinogen to angiotensin I. Angiotensin converting enzyme, found in the lungs, converts angiotensin I to angiotensin II. Angiotensin II increases peripheral vascular resistance directly and stimulates aldosterone secretion, resulting in increased reabsorption of sodium and water in the distal convoluted tubules. The afferent arteriole (choice A) carries blood from the interlobular arteries to the glomerulus. Filtration of blood occurs in the glomerulus, with the filtrate entering Bowman's capsule. The arcuate arteries (choice B) are branches of the interlobar arteries of the kidney. The arcuate arteries lie in the corticomedullary junction of the kidney and give rise to interlobular arteries, which enter the cortex of the kidney and supply the glomeruli. Kupffer cells (choice D) are found in the liver, along the sinusoids. They are phagocytic cells that are part of the reticuloendothelial system. The proximal convoluted tubule (choice E) is directly continuous with Bowman's capsule. Most of the resorption of the glomerular filtrate occurs in this part of the nephron.
46The correct answer is E. Any previously healthy person in the Southwestern United States who develops septic shock or severe pulmonary disease should be evaluated for plague. Plague is not an extinct disease, but is still encountered in sporadic cases in various places in the world, including Asia, Africa, parts of Europe, and the American Southwest. The causative organism is Yersinia pestis, which is endemic in many wild animal populations, and can be transmitted to humans either by direct contact or by arthropod bite. Human plague may take many forms, including pestis minor (mild lymphadenopathy); bubonic plague (prominent lymphadenopathy); pneumonic plague (as in this patient); and septicemic plague. The primary pneumonic form typically presents as described. Antibiotics are most effective if given within the first 24 hours, which can be problematic if medical staff do not suspect the disease. Since plague is rare in the United States, a high degree of clinical suspicion is required to make a rapid diagnosis and to institute timely treatment. If the diagnosis is missed, the mortality rate is quite high. Brucella abortus (choice A) causes brucellosis, characterized by undulating fever, lymphadenopathy, and hepatosplenomegaly. Clostridium perfringens (choice B) causes gas gangrene and gastroenteritis. Francisella tularensis (choice C) causes tularemia, associated with a spectrum of manifestations from an influenza-like syndrome to adenopathy with ulceration at the site of inoculation. Listeria monocytogenes (choice D) causes listeriosis. Infection during pregnancy may result in sepsis, abortion or premature delivery. Infection in the neonate may produce meningitis. In immunocompromised adults, either meningitis or sepsis may occur.
47The correct answer is D. Although electroconvulsive therapy (ECT) is highly efficacious in treating major depressions that are refractory to tricyclic antidepressants and selective serotonin reuptake inhibitors, it produces retrograde amnesia as its major side effect. Extrapyramidal symptoms (choice A) are commonly produced by acute administration of antipsychotic drugs, such as phenothiazines or butyrophenones, not ECT. Hearing loss (choice B) is not a common side effect of ECT. Mania (choice C) is not a recognized side effect of ECT. Rhabdomyolysis (choice E) does not generally occur with ECT when it is performed correctly, with the administration of skeletal muscle relaxants.
48The correct answer is B. The total lung capacity is the sum of the functional residual capacity and inspiratory reserve capacity. The easiest approach to this type of question is to construct a simple spirogram (see below) and fill in the values provided in the table. This approach eliminates the need to memorize formulas. The missing volume or capacity can be easily determined from the spirogram. The total lung capacity, functional residual capacity, and residual volume are often increased in the emphysematous lungs of patients with a long-term history of cigarette smoking. A inspiratory reserve volume B expiratory reserve volume C inspiratory reserve capacity D vital capacity E residual volume F functional residual capacity G tidal volume H total lung capacity
49The correct answer is D. The right ventricle forms most of the anterior wall of the heart and extends from approximately the right border of the sternum to approximately 2 inches to the left of the sternum at the level of the fourth intercostal space. The left atrium (choice A) forms the posterior wall of the heart. The only portion of the left atrium seen on the anterior surface of the heart is the left auricular appendage, which is at the level of the second intercostal space on the left. The left ventricle (choice B) forms most of the left border of the heart and the diaphragmatic surface of the heart. It forms the anterior wall of the heart in a region from approximately 2-3 inches from the left border of the sternum from the third to the fifth intercostal space. The right atrium (choice C) forms the right border of the heart. Its anterior surface is on the right side of the sternum from approximately the third rib to the sixth rib. The left lung (choice E) is displaced away from the sternum on the left side by the presence of the heart.
50The correct answer is E. Pemphigus vulgaris is associated with chronic, severe bullae formation on the skin and oral mucosa. Mucosal lesions are extremely rare in bullous pemphigoid. This can be used clinically to guide therapy, although a skin biopsy should be taken to confirm the diagnosis. Both diseases are characterized by formation of tender bullae that can rupture, leaving red, raw areas. Pemphigus vulgaris patients eventually become febrile and lose weight, and if untreated, most will die within one year. Bullous pemphigoid lesions tend to heal and the patients do very well. This prognostic difference is an important distinction in dermatologic medicine. Eosinophils within blisters (choice A) provide an important clue supporting bullous pemphigoid as the diagnosis which must be ascertained with histologic examination. The vesicles in pemphigus vulgaris mostly contain rounded acantholytic keratinocytes "floating" within. IgA deposits seen with immunofluorescence on the basement membrane (choice B) is characteristic of a third bullae-forming disease known as dermatitis herpetiformis. Vesicles form between the dermal-epidermal junction. The disease is associated with gluten sensitivity and celiac disease. IgG autoantibody activity (choice C) is common to both pemphigus vulgaris and bullous pemphigoid. Nikolsky's sign consists of separation of the epidermis upon manual stroking of the skin. Bullous pemphigoid is characterized by a negative Nikolsky's sign (choice D), but Nikolsky's sign is positive in pemphigus vulgaris due to the IgG-mediated destruction of intercellular bridges between keratinocytes.